Peripheral Artery Disease and Amputation: What You Need to Know—and How It’s Often Preventable
March 30, 2026
Peripheral Artery Disease (PAD) is commonly associated with leg pain during walking, but that’s only part of the story. When circulation to the legs and feet becomes severely limited and the condition goes untreated, PAD can turn into a serious, limb-threatening problem. In advanced cases, it can even result in amputation.
The encouraging news is that in many situations, limb loss can be avoided. With timely diagnosis, proper vascular care, and smart lifestyle changes, people with PAD can protect their legs—and their independence.
Understanding how PAD affects the body and knowing when to seek care can make a life-changing difference.
What Is Peripheral Artery Disease?
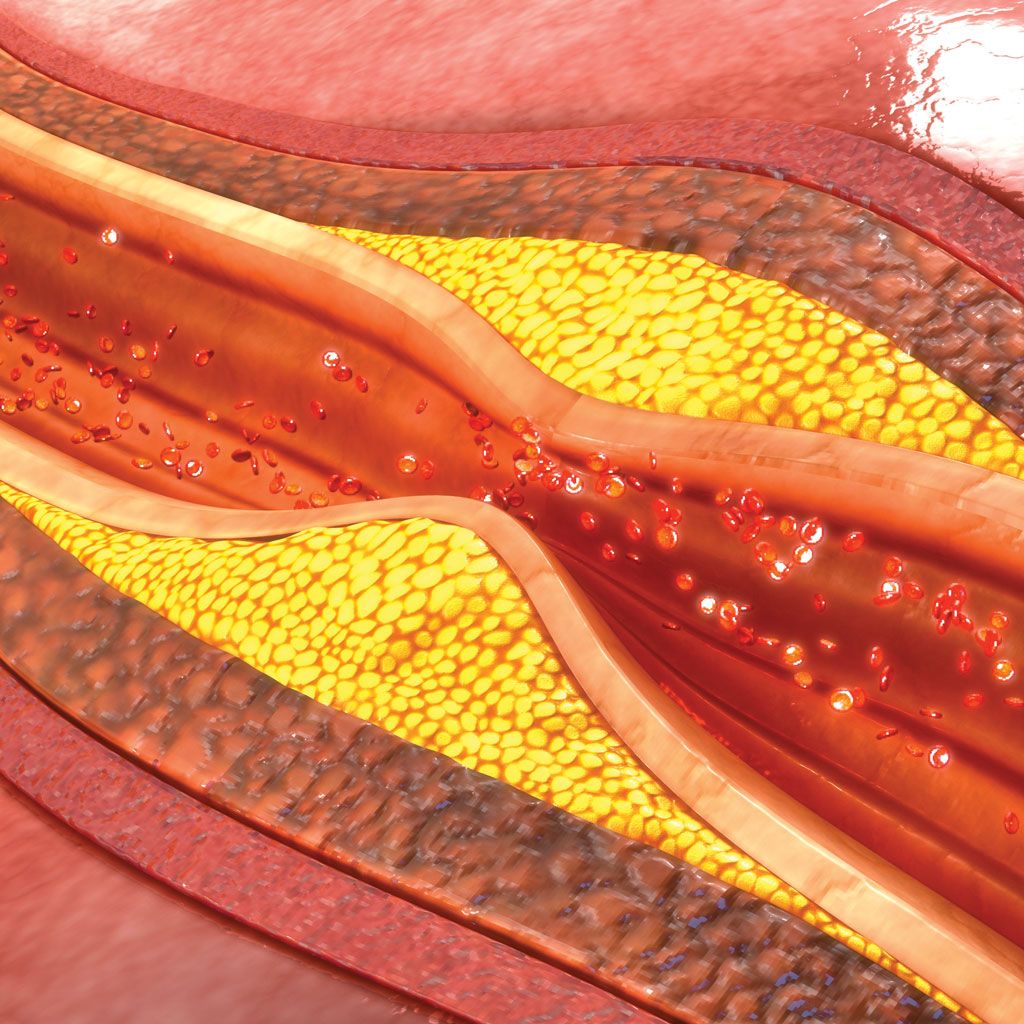
Peripheral Artery Disease develops when fatty plaque builds up inside the arteries that supply blood to the legs and feet. Over time, these arteries become narrowed or blocked, reducing the flow of oxygen-rich blood to muscles, skin, and other tissues.
PAD is a form of atherosclerosis and is closely associated with conditions and habits such as:
- Smoking
- Diabetes
- High blood pressure
- High cholesterol
- A history of heart disease or stroke
Some people notice symptoms early on, while others may have PAD for years without realizing it—until complications appear.
How Poor Circulation Can Turn Into a Serious Threat
The real danger of PAD lies in what happens when tissues don’t get enough blood to stay healthy and heal properly.
Weakened tissue
Reduced circulation makes the skin and muscles more fragile and more prone to injury.
Slow or non-healing wounds
Even small cuts, blisters, or pressure spots can linger when blood flow is poor. In people with diabetes, this risk is even higher.
Infection
Open wounds that don’t heal easily can become infected. When the blood supply is limited, the body has a harder time fighting infection and delivering antibiotics to the area.
Critical limb ischemia (CLI)
In advanced stages, PAD can progress to critical limb ischemia—a severe condition marked by ongoing pain, skin breakdown, and tissue death. At this point, urgent treatment is needed to save the limb, and in some cases, amputation is considered to prevent life-threatening complications.
Who Faces a Higher Risk of Limb Loss?
Not everyone with PAD will develop severe complications, but the risk is higher in people who have:
- Long-standing or poorly controlled diabetes
- A history of smoking or continued tobacco use
- Delayed diagnosis or untreated PAD
- Limited access to specialized vascular care
- Advanced symptoms such as rest pain, ulcers, or gangrene
The earlier PAD is identified and treated, the better the chances of avoiding serious outcomes.
Symptoms of PAD
PAD often sends warning signals. Don’t ignore symptoms such as:
- Leg pain or cramping during walking that improves with rest
- Coldness, numbness, or tingling in the feet or toes
- Sores or wounds on the legs or feet that heal slowly—or not at all
- Changes in skin color or texture, including shiny or thin skin
- Weak or hard-to-find pulses in the feet
If you notice any of these, a vascular evaluation can help determine the cause and the next steps to take.
How PAD-Related Amputation Can Be Prevented
Limb loss is not an automatic outcome of PAD. In many cases, a combination of medical treatment and lifestyle changes can slow the disease, improve circulation, and protect the legs.
Early testing and follow-up
Simple, noninvasive tests can evaluate blood flow in the legs and help confirm a diagnosis. Catching PAD early opens the door to more treatment options and better results.
Healthy lifestyle changes
Small, consistent changes can make a big impact, including:
- Quitting smoking
- Keeping blood sugar under control
- Managing cholesterol and blood pressure
- Participating in structured walking or exercise programs
These steps help improve circulation and reduce the risk of complications.
Medications
Your provider may prescribe medications to improve blood flow, reduce the risk of clots, and control conditions such as high blood pressure or high cholesterol that contribute to PAD.
Minimally invasive treatments, such as angioplasty
For moderate to severe PAD, minimally invasive procedures can restore blood flow and lower the risk of limb-threatening complications.
Angioplasty involves guiding a thin catheter to the narrowed area of an artery and inflating a small balloon to open it. In some cases, a stent (a small mesh tube) is placed to help keep the artery open. These procedures are typically done through a tiny incision, involve minimal downtime, and can significantly improve symptoms and support wound healing.
Ongoing foot and wound care
Regular foot checks and prompt treatment of any sores are especially important for people with PAD or diabetes. Addressing wounds early can prevent infection and more serious problems.
The Bottom Line: PAD Doesn’t Have to Mean Amputation
Peripheral Artery Disease is a serious condition—but with the right care, amputation is often preventable. Knowing the warning signs, understanding your risk factors, and getting timely treatment can protect your mobility and your quality of life.
If you’re experiencing leg pain, dealing with slow-healing wounds, or have risk factors for vascular disease, don’t put it off. Early action can make all the difference.
National Vascular Physicians specialize in diagnosing PAD. If an intervention is needed, NVP physicians can treat most conditions in our outpatient facility.
Contact us today to see how we can help! You deserve to feel good about your legs!



